
Simply put, lactose intolerance is the inability of an individual to digest lactose (milk sugar). This complication often leads to undesirable side effects. Lactose intolerance arises due to the deficiency of the lactase enzyme, which is responsible for the catalytic hydrolysis of the lactose into glucose that can be easily absorbed into the blood.
The problem of lacatse enzyme deficiency is referred to as hypolactasia. This is when the body cannot produce enough lactase enzyme to digest lactose. This causes lactose intolerance. To some extent, hypolactasia may be congenital. In such cases, the victims may not even be able to digest human milk. You should note that lactose intolerance is not milk allergy because it is not an immune response due to the presence of milk proteins.
May include flatulence, bloating, cramps, vomiting, rumbling stomach/stomach upsets, nausea, and diarrhea. Normally, most mammals cease lactase production after weaning because they do not need it then. However, humans continue to consume milk long after weaning even into their adulthood.
Some studies have shown that some human populations have developed lactase persistence into their adulthood, enabling them to digest the lactose in milk from cattle and goats. These symptoms are as a result of gas production in the small intestine. The lactose sugar cannot be absorbed directly through the walls of the small intestine because it is a disaccharide.
The sugar passes to the colon where the colon bacteria ferments it. The fermentation process produces large amounts of hydrogen, carbon IV oxide, and methane. The mixture of gases is responsible for all the symptoms manifested by a lactose intolerant individual.
The prevalence of lactose intolerance varies greatly with exposure to dairy products. Those who access dairy products much readily tend to be more tolerant to lactose. This is because the exposure encourages their bodies to continue producing the enzyme.
On the other hand, those who are less exposed to the dairy products tend to be more intolerant to the lactose because their bodies cease to produce the lactase enzyme. However, there are exceptions to this observation and may be associated to genetics.
Lactose intolerance arises due to deficiency of lactase enzyme. The deficiency of the enzyme can be traced to the following causes
Before the advancement of technology to produce lactose free dairy products and soybean derived baby formulas, the babies born with congenital lactose deficiency never survived.
Listed below are the tests you can carry out to confirm lactose intolerance.
By far, this is the most accurate test for lactose intolerance. It involves consumption of about 20 grams of lactose made into a solution after fasting for more than 12 hours, preferably overnight.
Since the colon bacteria will metabolize the substrate to produce the gas mixture discussed previously, the gas will be traced in the person’s breath by doing a chromatography test. The procedure takes between two to three hours to finish.
This test is best suited for diagnosing lactose intolerance in infants. The infant is given lactose to drink and the stool tested. Those who are tolerant will digest the lactose and absorb it. Those who are intolerant to lactose will have the lactose reach the colon.
Here, the colon bacteria will metabolize the lactose to produce the mixture of gases. This mixture of gases produces acidity in the stool. The confirmation of acidity in the infant stool after consuming lactose is a confirmation of intolerance.
This test identifies traces of sugar in the stool. It is not a very reliable means of identifying lactose intolerance in individuals due to the chemical changes that take place to the lactose in the intestines.
Intestinal biopsy can confirm lactose intolerance in an individual who has elevated levels of hydrogen in their breath after consuming lactose. By using the gastrointestinal endoscopy equipment, the medical practitioner can be able to identify the deficiency of lactase enzyme in the duodenum.
The blood sugar levels of the lactose tolerant individuals will show a significant boost after consuming lactose. This is a different observation from the lactose intolerant individuals who will remain level even after consuming lactose. This is because the tolerant individuals are able to break down the complex sugar (lactose) into simple glucose that the body can absorb.
The intolerant individuals are not able to break down the complex sugar into glucose. The lactose broken down into glucose is responsible for the spike in blood sugar. After fasting overnight, blood is drawn and tested for blood sugar then the individual is given lactose to ingest. The blood test is repeated after intervals of half an hour, then one-hour, two hours, and three hours.
If the individual is unable to absorb the lactose, there will be insignificant rise in blood sugar.
Lactase persistence in adults is controlled by polymorphic allele in the genes. The procedure involves extraction of DNA material from the blood or saliva of the individual.
Following a matching band of colors, it will be possible to detect whether the person is lactose intolerant or not.
Lactose is a water-soluble milk sugar. It is often found in the whey portion of the milk when making cheese. The following dairy products contain lactose
It is always important to read the labels of the commonly used non-dairy food products as manufacturers often add dairy products to them. Some of the non-dairy products you may find to contain lactose include the following:
The best medicine for lactose intolerance is to avoid lactose at all costs. If the route of avoidance is out of question, supplementation may be necessary. It is possible to industrially produce lactase by using Aspergillus spp. fungi. You can obtain the β-galactosidase enzyme as a tablet supplement over the counter without prescription.
One needs to take the supplement at the same time they are taking the lactose-laden food for the supplement to be effective. It works best in an acidic environment; however, too much acid can denature it and render it useless.
Video on natural ways to deal with lactose intolerance (source: Natural Cures)
We have looked at lactose intolerance, so we know what it is and its causes. We have also seen the various ways victims of lactose intolerance can try to reduce the impact of the problem.
The lactose content is expressed as a percentage of the whole volume. The value varies from one milk sample to the next depending on various factors
Once you have run all the tests and recorded the volume of lactose solution used in every sample, you can determine the value of lactose content in each sample as follows:
Volume of lactose solution used in the control sample = x ml
Volume of lactose solution used in the milk sample = y ml
Percentage lactose (milk sample) = {(x-y)*0.05}/2.5
Where: 0.05 is the % conversion factor for the lactose content and 2.5 is the dilution factor (0.1) multiplied by the diluted sample used in the test (25ml).
This section of the article was contributed by Josef Michael Kienböck of Direct Sens. Direct Sens is a university-connected venture with a strong scientific basis on life science technologies. You can see their projects here: http://www.directsens.com/lactosens/
Milk is a very rich source of lactose, which causes lactose intolerance to over 70% of adult population globally. Lactose intolerance affects people of all ethnicities/races. Lactose content determination for product labeling purposes is critical owing to the serious nature of lactose intolerance.
For instance, Virtual Medical Center indicates the following: Primary lactose intolerance affects between 7 - 20% Caucasians, 65 to 75% African descent, 90% in certain Asian populations and about 70% Australian/Aboriginal populations.
Putting these figures into perspective can be very depressing, especially when considering dairy products as a means to fight world hunger and malnutrition.
Increasingly, many people are pushing for dairy products with reduced lactose content. Through technology, several advances have been made.
For instance, fermented products such as yoghurt and cheeses have proven very popular. This is because they do not elicit similar reactions as fresh milk in people with lactose intolerance.
A similar story cannot be said about fluid milk. Fluid milk forms the bulk of dairy products consumed globally by volume.
But there is a problem,
Fluid milk naturally has high content of lactose making it unsuitable for many who are lactose intolerant.
Determination of lactose content is usually a tedious process involving a series of meticulous steps. The process is often expensive and time consuming. Most labs do not have the sophisticated equipment required for these tests (HPLC or GC) hence many processors often opt out.
There needs to be a cheap, accurate and reproducible method of determining and controlling the lactose content in fluid milk and other dairy products.
Luckily, there is a new rapid and relatively cheap lactose content determination method that can be adopted for both industrial and artisanal use.
LACTOSENS® Assay: A computerized rapid, accurate and cheaper lactose content determination method for dairy products.

Imagine, if you could measure the precise residual lactose level in your dairy products in real-time - at every stage of production and with a sensitivity of 0.01%.
LACTOSENS®, based on amperometric biosensor technology, is the ideal solution for process monitoring and quality control. It provides a quick and efficient route to market and shortening lead times in the booming lactose-free segment.
With the globalization of dairy markets, “lactose-free” has become a solution to meet the needs of over 70% of the world’s population!
Infants are born with the ability to produce lactase, but with increasing age the production of lactase reduces or ceases.
In order to avoid inconveniences resulting from lactose non-digestion, many consumers are turning to “lactose-free” dairy products. This allows them to commonly use milk as an important source of protein, minerals and vitamins.
With this increasing importance of “lactose-free” products, the relevant threshold for “lactose-free” labeling has been revised from the former 0.1g/ml to the more stringent standard of 0.01g/ml.
This readjustment to the lower threshold is aimed at people with severe lactose intolerance. The adjustment presents even a bigger challenge for dairies. Existing methods for precise control and verification of a 0.01% lactose threshold are quite laborious, slow and expensive, especially when not executed in-house.
Thus, dairies may have to wait for days to get a result for product release – or release batches based on “typical” results. This means such dairies will not have traceable batch-specific concentration data available for all productions.
The LACTOSENS® 0.01% assay – recently validated against HPLC - here opens a unique access for dairies and even processing dairy farmers to a fast and precise method for lactose concentration measurement.
The test involves a direct assay on a biochip that very specifically measures lactose in mere minutes in milk and dairy products as yogurt, sour cream, fresh cheese and mozzarella.
The graph below shows how the accuracy of LactoSens compares to the HPLC for lactose content determination.
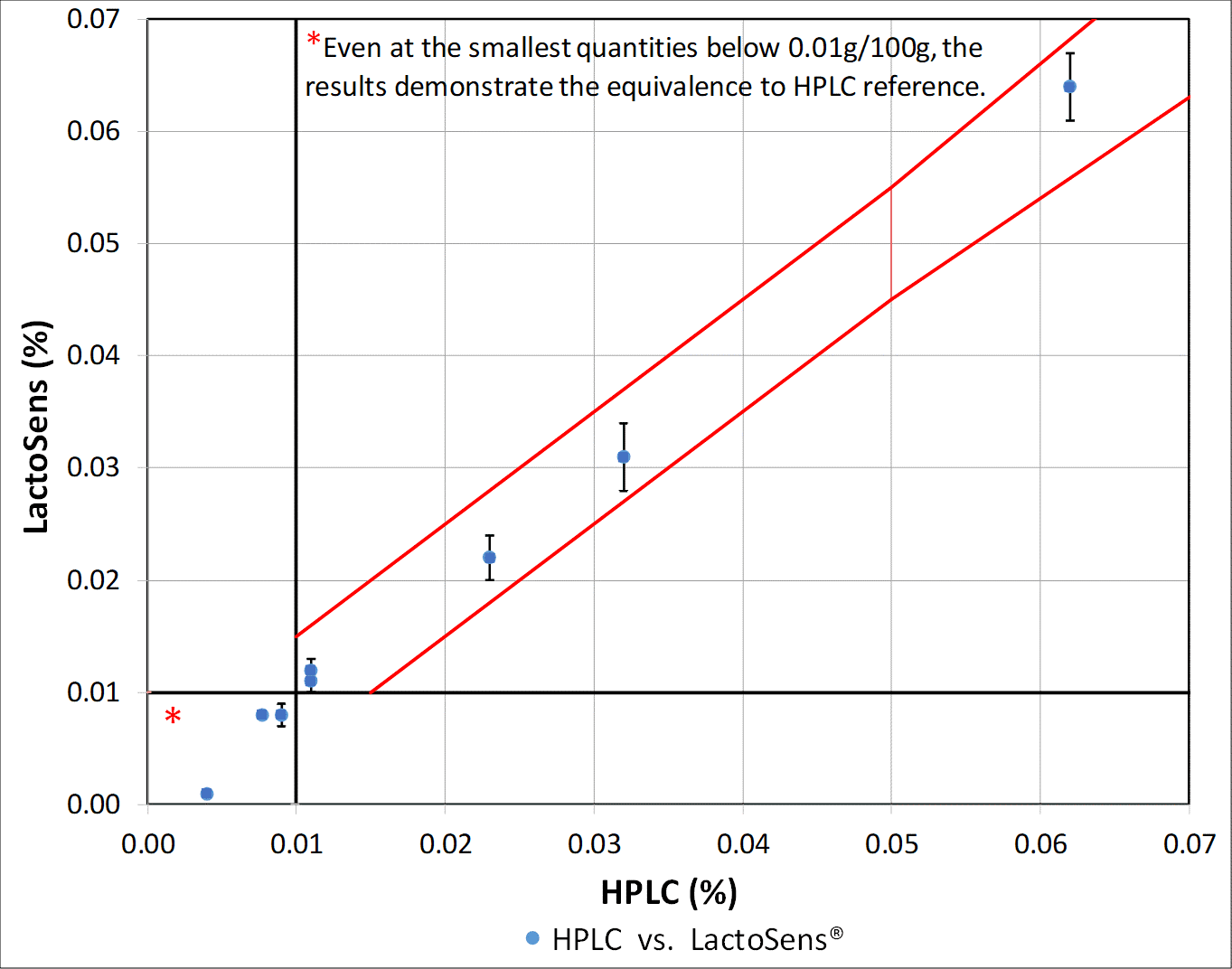
What’s the secret functional principle of this fast and precise LACTOSENS® biosensor?
You can check out the LactoSens product documentation for more details.
How to operate the LACTOSENS® machine for lactose content determination in dairy products
LACTOSENS® TEST - SO SIMPLE & FAST
Produces results in < 1 minute
The video below illustrates how LACTOSENS® machine is used to determine the lactose content of dairy products
Certification by NordVal International
The LACTOSENS® trace analysis detection is so precise, that the NordVal International Institute of the Technical University of Denmark has certified the LACTOSENS® biosensor - in the sensitive range between 0.1% and 0.008% - as equivalent to the lactose reference method HPLC:
The high-performance liquid chromatography requires expensive equipment and qualified personnel.
Control studies were done at two ISO 17025 accredited laboratories. The results validated the LACTOSENS® biosensor against the HPLC method in ruggedness, specificity of detection, stability testing and batch-to-batch variation (traceability), limit of quantification, precision and internal reproducibility (reliability).
This NordVal validation study confirms the LACTOSENS® biosensor as unique rapid lactose test. It detects lactose at levels of 0.008% and produces comparable results to the HPLC method.
You can find the NordVal Certificate for LACTOSENS® here.
'Lactosens is ideal for both process control and product release in the dairy industries,' explains Jes Jensen, Director of Testing and Equipment at Chr. Hansen. 'It is the fastest and easiest method available, revolutionizing the way in which the dairy industry analyzes lactose.'
All customer orders from different parts of the world are fulfilled through Chr. Hansen exclusively. Chr, Hansen is a leading well-known dairy specialist with sufficient sales force and offices covering all global markets.
You can get in touch with them to inquire about LACTOSENS® https://www.chr-hansen.com/en/contact.


Comments