
Bacterial zoonoses pose a greater health risk to humans. Viral zoonoses compound the risk since they spread fast and are hard to contain. On the other hand, other zoonoses like those of parasitic origin may not show any clinical symptom in their immediate host. When people consume products from such hosts, they get infected.
One perfect example is taeniasis, which does not show any clinical symptom in cattle. However, when they get into the human host, the worm multiplies rapidly and reach an attacking threshold. It can cause damaging effects on the host since the human victims feel ashamed to admit that they have worms.
We are going to look at some viral, rickettsial and parasitic zoonoses of economic importance in the food industry. We will also look at their symptoms, diagnosis, treatment, and control measures.
Viral zoonoses are acute and affect all warm-blooded animals and humans. The major characteristics of these diseases include hyper-excitability, paralysis, and death.
They are caused by an RNA virus that is very sensitive and will be inactivated by:
It is however resistant to freezing. Freezing it actually preserves it.
When a viral zoonose occurs in humans or animals, it will cause acute symptoms.
Carnivores tend to be the natural hosts of viral diseases. Infected animals have very high concentration of the virus in their saliva before any clinical sign of infection occurs.
Viral zoonoses have a global presence.
Viral zoonoses spread through bites from the natural host or contact with body fluids from an infected warm-blooded host.
The GIT may also be a route though there aren’t any documented cases.
The virus is introduced through a bite. It into the peripheral nerve and moves to the central nervous system through motor action.
The signs are typically manifested in dogs.
Onset of the disease varies with the site of the bite. Incubation period takes long period (3 – 8 weeks on average though it can be as short as 10 days or as long as 6 months).
The symptoms of the disease takes two forms in dogs:
This is the most common form of rabies in carnivores. It appears in three stages:
The dog starts with the prodromal phase but skips the excitable phase. It goes straight to paralysis phase.
Rabid cattle are furious. They bellow a lot and are aggressive but they do not bite. Paralysis and death follows eventually.
Cattle are dead-end hosts of rabies because they do not transmit it to any other host.
People get the disease from a carnivore’s bite. Incubation period is between 30 – 60 days, which also depends on the site of the bite.
Initial symptoms are usually general, e.g. headache, general malaise, slight fever, nervousness, anxiety, and a tingling sensation at the bite site.
After these signs, the characteristic symptoms for humans will set in. They include:
Confine animals suspected to have rabies. After their death, use their brain for diagnosis (check the negri bodies).
You can also do serological tests.
In humans, the patient’s history is very important in diagnosis.
Once the disease has started in animals, it is untreatable. It will progress until the host dies.
In humans, give repeated vaccinations as soon as you realize the patient is suffering from rabies.
This disease was first diagnosed in Naivasha in 1931. It caused abortions in sheep and had high mortality rates of up to 95 percent.
In 1951, a similar syndrome occurred in South Africa in sheep. People who came into contact with the sick animals also got sick. One hundred people died and about 100 000 sheep and cattle were infected.
The disease then spread to other parts of Africa. No incident of this disease has ever been reported outside Africa.
This disease is caused by the insect-borne arbovirus. This virus has high affinity for the liver hence it majorly affects the liver.
In animals, mosquitoes are majorly responsible for the transmission, though other insects are suspects as well.
People can be infected by handling aborted material from sick animals. Sick animals also shed the virus in milk, which becomes a route of transmission in humans. Human to human transmission is not documented.
Majorly associated with monkeys. Cause haemorrhagic syndrome in humans.
Common in Africa, South America, and several other Asian countries
Caused by yellow fever virus. Natural hosts are primates. The virus is transmitted by insects from the primates to humans.
Forest workers and hunters are more susceptible.
The disease is apparent in animals but humans get severe symptoms such as:
It is caused by a primate-associated virus. Lab workers are mostly affected and they contact the virus through aerial contamination.
The disease is inapparent in animals but people experience acute fever, vomiting, and diarrhoea. Lymphadenopathy (swollen lymph nodes), haemorrhage, and death is quite common.
Take a lot of care when handling patients
Lassa virus is responsible for causing Lassa fever. The virus is common in rodents and people contact it from them via aerial contamination.
Ebola is a very severe and fatal disease in humans. It is associated with primates and is caused by the ebola virus, which has many strains including:
It was first confirmed in the Democratic Republic of Congo (DRC) but has since spread to other parts. In DRC, it occurs mainly as the Zaire sub-type.
It is transmitted through contact with the body fluid of an infected patient.
Rickettsial zoonoses, a group of vector-borne illnesses caused by Gram-negative obligate intracellular bacteria, are transmitted by ticks, fleas, lice, and mites. The advancement of molecular diagnostic tools has led to the discovery of numerous rickettsial species, making rickettsioses the most common emerging/reemerging zoonoses globally.
Scrub typhus, which causes significant disease burden, remains the most crucial rickettsial infection globally and is predominantly found in the "tsutsugamushi triangle" geographic region. This triangle extends from northern Japan and Eastern Russia in the north to northern Australia in the south and Pakistan in the west and causes almost a million cases annually, with practically a billion individuals at risk.
Here, we'll discuss a few selected rickettsial zoonoses, their aetiology, diagnosis, tretment and containment measures.
This is a food-borne disease as well as a zoonose. It is common in most parts of the world.
In animals, it causes abortions and in humans, it causes serious disease. It is a professional hazard for people dealing with livestock and those handling raw animal products.
Ticks are the main carriers and the pathogen will be found in the aborted material. It is also found in the placenta of cattle, sheep, and goats as well as in milk of these animals.
It is caused by a rickettsia microorganism Coxiellae burnettii.
People get the disease as a professional hazard when they inhale or contact a sick animal and/or the aborted material.
Consuming contaminated milk and milk products is also a route of transmission.
Human to human transmission has not been recorded. However, the organism has been extracted from milks of mothers who have recovered from the disease.
Incubation period lasts 2 – 4 weeks. Observable symptoms include:
Do serological tests for confirmation of the organism.
Isolate the microorganism from the aborted material.
Typhis fever affect both humans and animals, especially dogs. They are transmitted by ticks and fleas.
Dogs and monkeys do not get serious disease.
In humans, the patient may experience high fever, joint pains, muscle pain, swellings at the bite sites that may progress into ulcers.
Lymph nodes that are proximal to the bite site will swell.
Spontaneous recovery usually occur.
|
Antigenic group |
Disease caused |
Active species |
Vector |
Immediate host |
Where found |
|
Anaplasma |
Human anaplasmosis |
Anaplasma phagocytophilum |
Tick |
Small mammals, rodents, deer |
Primarily United States, worldwide |
|
Ehrlichia |
Human ehrlichosis |
Ehrlichia chaffeensis |
Tick |
Deer, wild and domestic dogs, domestic ruminants, rodents |
Common in United States, possibly worldwide |
|
Neoehrlichia |
Neoehrlichiosis |
Neoehrlichia mikurensis |
Tick |
Rodents |
Europe, Asia |
|
Neorickettsia |
Sennetsu fever, neorickettsiosis |
Neorickettsia sennetsu |
Trematode (ingestion) |
Fish |
Japan, Malaysia, possibly other parts of Asia |
|
Scrub typhus |
Scrub typhus |
Orientia tsutsugamushi |
Larval mite (chigger) |
Rodents |
Asia-Pacific region from maritime Russia and China to Indonesia and North Australia to Afghanistan |
|
Spotted fever |
Rickettsiosis |
Rickettsia aeschliman- |
Tick |
Unknown |
South Africa, Morocco, Mediterranean littoral |
|
African tick-bite fever |
R. africae |
Tick |
Ruminants |
Sub-Saharan Africa, West Indies |
|
|
Rickettsialpox |
R. akari |
Mite |
House mice, wild rodents |
Countries of the former Soviet Union, South Africa, Korea, Turkey, Balkan countries, United States |
|
|
Queensland tick typhus |
R. australis |
Tick |
Rodents |
Australia, Tasmania |
|
|
Mediterranean spotted fever or Boutonneuse fever |
R. conorii |
Tick |
Dogs, rodents |
Southern Europe, southern and western Asia, Africa, India |
|
|
Cat flea rickettsiosis |
R. felis |
Flea |
Domestic cats, rodents, opossums |
Europe, North and South America, Africa, Asia |
|
|
Far Eastern spotted fever |
R. heilong- |
Tick |
Rodents |
Far East of Russia, Northern China, eastern Asia |
|
|
Aneruptive fever |
R. helvetica |
Tick |
Rodents |
Central and northern Europe, Asia |
|
|
Flinders Island spotted fever, Thai tick typhus |
R. honei, including strain "marmionii" |
Tick |
Rodents, reptiles |
Australia, Thailand |
|
|
Japanese spotted fever |
R. japonica |
Tick |
Rodents |
Japan |
|
|
Mediterranean spotted fever-like disease |
R. massiliae |
Tick |
Unknown |
France, Greece, Spain, Portugal, Switzerland, Siciliy, central Africa, Mali, and Argentina |
|
|
Mediterranean spotted fever-like illness |
R. monacensis |
Tick |
Lizards, possibly birds |
Europe, North Africa |
|
|
Maculatum infection; Tidewater spotted fever; American boutonneuse fever |
R. parkeri |
Tick |
Rodents |
North and South America |
|
|
Tickborne lymphadenopathy, Dermcentor-borne necrosis and lymphadenopathy |
R. raoultii |
Tick |
Unknown |
Europe, Asia |
|
|
Rocky Mountain spotted fever |
R. rickettsia |
Tick |
Rodents |
North, Central, and South America |
|
|
North Asian tick typhus, Siberian tick typhus |
R. sibirica |
Tick |
Rodents |
Russia, China, Mongolia |
|
|
Lymphangitis-associated rickettsiosis |
R. sibirica mongolotimonae |
Tick |
Rodents |
Southern France, Portugal, China, Africa |
|
|
Tickborne lymphaden- |
R. slovaca |
Tick |
Lagomorphs, rodents |
Southern and eastern Europe, Asia |
|
|
Typhus fever |
Epidemic typhus, sylvatic typhus
Murine typhus, fleaborne typhus |
R. prowazekii
R. typhi |
Human body louse, flying squirrel ecto- |
Humans, flying squirrels
Rodents |
Central Africa; Asia; Central, North, and South America
Tropical and subtropical areas worldwide |
Table Source: CDC
Psittacosis is derived from the Greek word psittacus, which means parrot. Te disease is associated with parrots. Ornithosis means it is associated with birds.
The disease is simply referred to as psittacosis in humans regardless of the source. People get it by direct contact with sick birds.
The causative organism is Chlamydia psittaci.
The responsible chlamydia is a common flora in birds hence there only needs to be a change in the physiological conditions of the bird for the organism to attack.
Stressed birds will develop the disease. Stress can arise from different sources including transportation or noise. Affected birds will exhibit the following symptoms:
During the active stage of the disease, the microorganism is highly concentrated in the faeces, which becomes the major source of contamination.
People get the disease through contact with sick birds during the active stage of the disease.
Human to human transmission occurs, though not very common. The chlamydia can be air-borne.
Incubation usually takes between 1 – 2 weeks after exposure. The symptoms then commence as a typical pneumonia. Observable symptoms include:
Conduct routine checks in animals. Isolate sick birds for confirmation.
In humans, perform lab tests at the hospital.
In birds, do prophylactic treatment (give them oxytetracycline)
People should get prescription form the hospital. Usually, oxytetracycline is given.
Parasitic zoonoses are diseases caused by parasitic organisms that can be transmitted from animals to humans. Parasites such as protozoa, helminths, and arthropods can cause a range of illnesses in humans, from mild discomfort to severe disease. The most common parasitic zoonoses are toxoplasmosis, malaria, leishmaniasis, giardiasis, and cryptosporidiosis.
These diseases are usually transmitted to humans through contact with contaminated animal feces, contaminated food or water, or through the bites of infected insects and other vectors. In addition, people who work with animals, such as farmers, veterinarians, and animal handlers, are at increased risk of contracting parasitic zoonoses.
In this post, we are going to take a loook at a few parasitic zoonoses of importance in food.
Parasitic zoonoses are associated with meat. Psychrozoonoses require more than one vertebrate host to cause a disease.
Adult parasite (tapeworm) causes taeniasis while the larval stage causes cysticercosis. The adult stage is usually hosted by humans while the larval stage is found in animals (especially the domesticated ones).
The intermediate host is domestic animals like cattle and shoats (sheep and goats).
There are two prominent species of the tapeworm:
Cysticercosis in cattle is attributed to Cysticercus bovis (bovine) and Cysticercus cellulosae (pigs). Wild animals can also get Cysticercus bovis.
People can harbour both the larval and adult stages of Taenia solium. Humans are the immediate and permanent host of the worm. Human to human transmission does not occur.
Taenia solium eggs are transferred to other hosts through food.
Life cycle of Taenia spp. worm
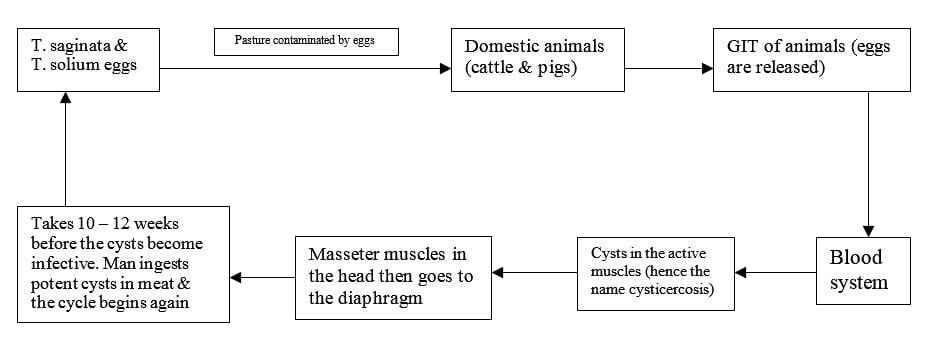
The life cycle of these two worms can begin anywhere within the cycle.
Analyse the stool for the eggs in humans.
In animals, conduct post-mortem tests and evaluate the cyst count. If the cyst count is less than 10, the meat is not condemned but sold under instruction. If the cyst count is greater than 20, condemn the meat.
In animals, the disease is not treated as they do not show clinical signs.
People should undergo regular deworming to eradicate the worm.
Hydatidosis is caused by hydatid cyst. The larval stage affects both humans and animals.
Echnococcosis is caused by two strains of echnococcus that inhabit dogs. The two strains are:
Humans are dead-end hosts for this parasite because dogs do not feed on human viscera.
Life cycle of the hydatid parasite
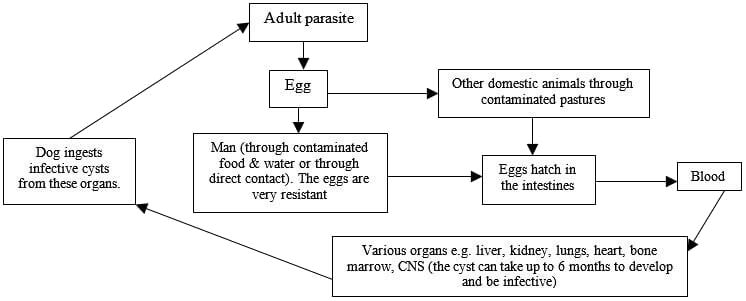
Other domestic animals may have the cyst in the internal organs but do not show any clinical signs.
|
Adult host |
Definitive host |
Organs affected |
Larval stage |
Intermediate host |
Organs affected |
|
T. saginata |
Man |
Intestines |
C. bovis |
Shoats & cattle |
Active muscles (e.g. tongue, diaphragm |
|
T. solium |
Man |
Intestines |
C. cellulosae |
Pigs |
Muscles |
|
Echnococcus |
Dog |
Intestines |
Hydatid cyst |
Humans & domestic animals |
Soft organs like liver |
This is a protozoan disease that affect all domestic animals. The infection is critical when the infection enters the cat because the cat hosts the infective stage of the disease.
The causative protozoan is Toxoplasma gondii.
The cat being the definitive host of the microorganism sheds the oocytes through the faeces. The oocytes sporulate once they come into contact with air.
Humans get the infection through the spores since they have a close association with cats. They can get into contact with the spores through:
Symptoms usually vary with age.
In animals, examine the faecal sample for the oocytes.
In humans, perform serological tests.
Trichinellosis is a parasitic zoonotic disease that is directly transmitted from animals to humans. The causative organism is a nematode called Trichinella spiralis.
The disease majorly occurs in the northern hemisphere. It is very prevalent in Alaska and places where people love wild boar and bear meat.
Horses also get the disease. Dogs, cats, and other carnivores also get the disease but they may not transmit it to humans.
The disease undergoes a similar cycle in humans as in animals.
People get the cyst from boar/bear/horse meat. When the cyst gets into the stomach, it vegetates and grows into an adult. It then passes into the intestines where it lays eggs.
Immature larvae will get into the blood and then pass into the muscles.
This disease is majorly transmitted through garbage and feeding. Some of the most common routes of transmission include:
When the nematode is still in larval stage, the patient may experience the following:
The adult parasite resides in the stomach. The sick animal will show the following signs:
Examine the faecal sample for the eggs of the parasite.
Regularly deworm the animals and people
Break the cycle of the nematode to discontinue infection cycle.


Comments